A comprehensive review of how VNS devices restore energy and vitality by addressing the nervous system dysregulation that drives persistent tiredness, with expert rankings of the top 4 certified options.

Chronic tiredness is estimated to affect more than one in three adults worldwide. This makes them among the most common yet most misunderstood health complaints in modern medicine.
Here’s why:
Unlike ordinary tiredness that resolves with a good night’s sleep, chronic tiredness reflects a fundamental dysfunction of the autonomic nervous system.
It disrupts cellular energy production, immune regulation, and the body’s capacity to recover from normal daily activity.
Recent neuroscience research suggests that vagus nerve dysfunction may contribute significantly to persistent tiredness in many individuals, alongside mitochondrial impairment, chronic low-grade inflammation, disrupted sleep architecture, and hormonal dysregulation.
And the mechanism is relatively straightforward:
When this primary parasympathetic nerve shows reduced activity, the body may lose its capacity to:
- Shift out of fight-or-flight mode
- Block inflammatory signalling
- Restore cellular energy reserves
- Achieve the deep restorative states that genuine recovery requires
This guide examines the relationship between vagus nerve function and chronic tiredness. It evaluates the leading vagus nerve stimulation (VNS) devices that may help restore autonomic balance, energy, and functional capacity.
Symptoms of Chronic Tiredness
Chronic tiredness is characterised by persistent, unrefreshing exhaustion that is disproportionate to activity level and not adequately explained by lifestyle factors alone. It often coexists with additional autonomic and inflammatory symptoms. Common manifestations include:
Energy and Physical Symptoms
- Profound exhaustion that sleep does not resolve
- Significant reduction in physical stamina compared to the previous baseline
- Muscle weakness, heaviness, or aching without exertion
- Post-exertional malaise, symptom worsening lasting 12 to 48 hours after mild activity
- Unrefreshing sleep despite adequate sleep duration
- Morning exhaustion despite having slept through the night
Cognitive Symptoms
- Brain fog, difficulty thinking clearly, concentrating, or processing information
- Slow word retrieval and reduced verbal fluency
- Short-term memory lapses affecting daily function
- Difficulty making decisions or sustaining attention
- Mental tiredness that arrives far sooner than physical tiredness
Autonomic and Inflammatory Symptoms
- Hypersensitivity to light, sound, or temperature
- Disproportionate tiredness following stress, infection, or emotional exertion
- Persistent low-grade feelings of illness or malaise
- Gastrointestinal symptoms, including bloating, nausea, and irregular motility
- Heart rate variability (HRV) that is measurably low even at rest
- Dizziness or lightheadedness when standing or after prolonged sitting
Sleep and Circadian Symptoms
- Difficulty falling asleep despite exhaustion
- Frequent nocturnal waking or non-restorative sleep cycles
- Irregular sleep-wake cycles and difficulty maintaining a consistent rhythm
- Excessive daytime sleepiness that does not respond to rest
- Feeling wide awake at night and most exhausted during the day
Immune and Systemic Symptoms
- Increased susceptibility to infections and prolonged recovery from illness
- Persistent low-grade inflammation markers on blood testing
- Swollen lymph nodes or recurring sore throat without active infection
- Temperature dysregulation, feeling unusually cold or overheated
- Tiredness that worsened following a viral illness and never fully resolved
The functional impact extends far beyond tiredness itself. Persistent tiredness forces people to withdraw from work, social life, exercise, and meaningful daily activity. It is frequently dismissed by conventional medicine, misattributed to depressive states or deconditioning, and left without effective therapy. This leaves millions of people to manage their lives around exhaustion rather than recovering from it.

Chronic Tiredness Self-Assessment
Evaluate the symptoms you experience with regularity:
Energy Patterns
- Tiredness that is present even after 7 to 9 hours of sleep
- Energy levels that crash after mild physical or mental activity
- A pattern of boom and bust, feeling slightly better, then significantly worse
- Morning exhaustion that doesn't lift for several hours after waking
- Energy that is unpredictable from day to day without a clear cause
Cognitive Function
- Noticeable brain fog affecting work or daily tasks
- Difficulty holding focus for more than 20 to 30 minutes
- Forgetting words, names, or recent events more than is typical
- Feeling mentally drained well before the day is over
- Once easy tasks now feel effortful and slow
Recovery Capacity
- Exercise or even light exertion triggers multi-day tiredness flares
- You need significantly more rest than others to perform at the same level
- You feel worse after stress rather than recovering once it passes
- Sleep does not restore your energy the way it once did
- Your body takes longer to recover from colds, infections, or travel
Nervous System Signals
- You feel wired but tired, exhausted yet unable to switch off
- Your resting heart rate is elevated or irregular
- You have low HRV readings on a wearable tracker
- You feel physically tense even when mentally resting
- Small stressors produce a disproportionate physical response
Functional Capacity
- Tiredness limits your ability to work, exercise, or socialise consistently
- You regularly cancel plans due to insufficient energy
- You rely on caffeine, stimulants, or willpower to function through the day
- You have modified your life significantly to manage your energy levels
- You have pursued multiple interventions with incomplete or no relief
Health History
- Tiredness began or worsened following a viral illness, surgery, or major stress event
- Blood tests, thyroid panels, and iron levels have come back normal
- You have been told your tiredness is stress-related or psychological, without clear evidence
- Conventional solutions, including sleep hygiene, exercise, and supplementation, have not resolved your tiredness
- The tiredness has persisted for more than three months
If you identify with several features across the energy, recovery, and nervous system categories, autonomic nervous system dysregulation may be a significant contributing factor to your tiredness.
In many individuals, impaired vagal tone and chronic sympathetic activation maintain a physiological state. This makes genuine rest and recovery structurally impossible, regardless of how much sleep is obtained.
Vagus nerve stimulation may be worth discussing with your health professional as an adjunctive approach.

The Vagus Nerve Connection
What Is the Vagus Nerve?
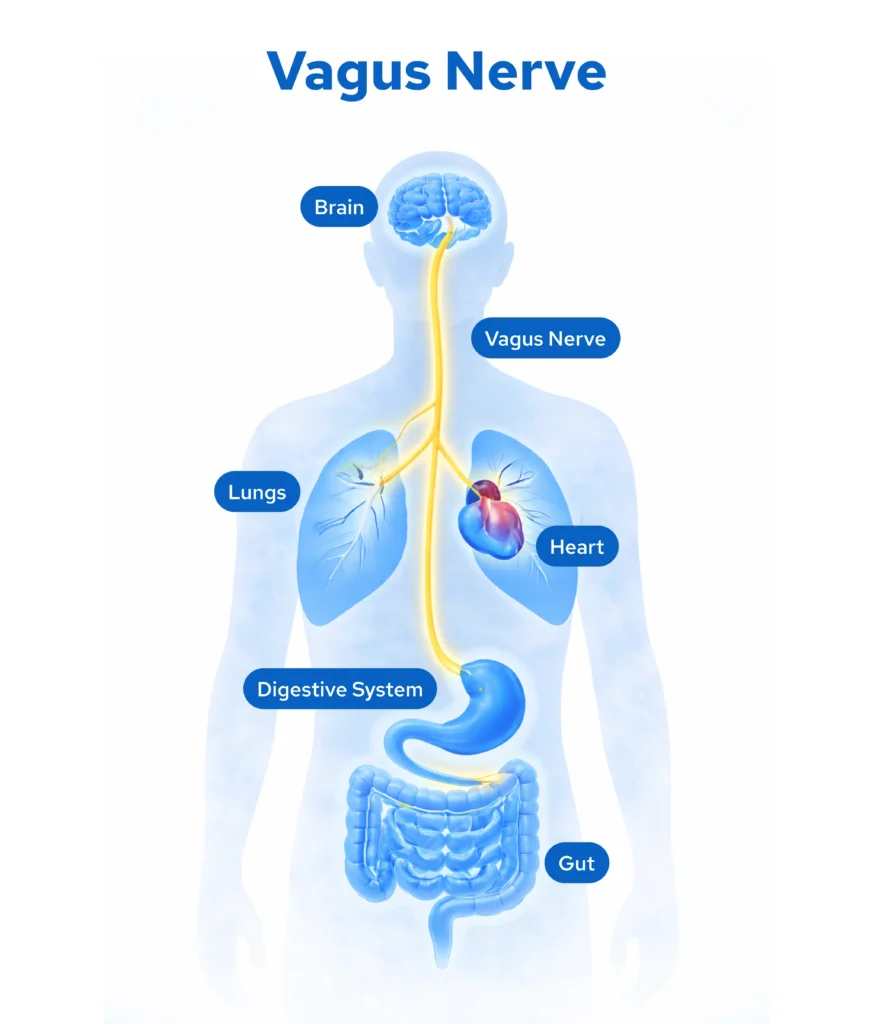
The vagus nerve (cranial nerve X) is the longest and most complex nerve of the autonomic nervous system. It originates in the medulla oblongata and projects through the neck to innervate the heart, lungs, and gastrointestinal tract.
It mediates the body’s most essential restorative functions:
- Cardiovascular regulation, heart rate control and baroreflex integration
- Respiratory pattern modulation and breathing efficiency
- Gastrointestinal motility, digestion, and nutrient absorption
- Inflammatory reflex pathway, the cholinergic anti-inflammatory pathway
- Sleep architecture regulation and circadian rhythm synchronisation
- Mitochondrial function and cellular energy metabolism
- Immune surveillance and cytokine regulation
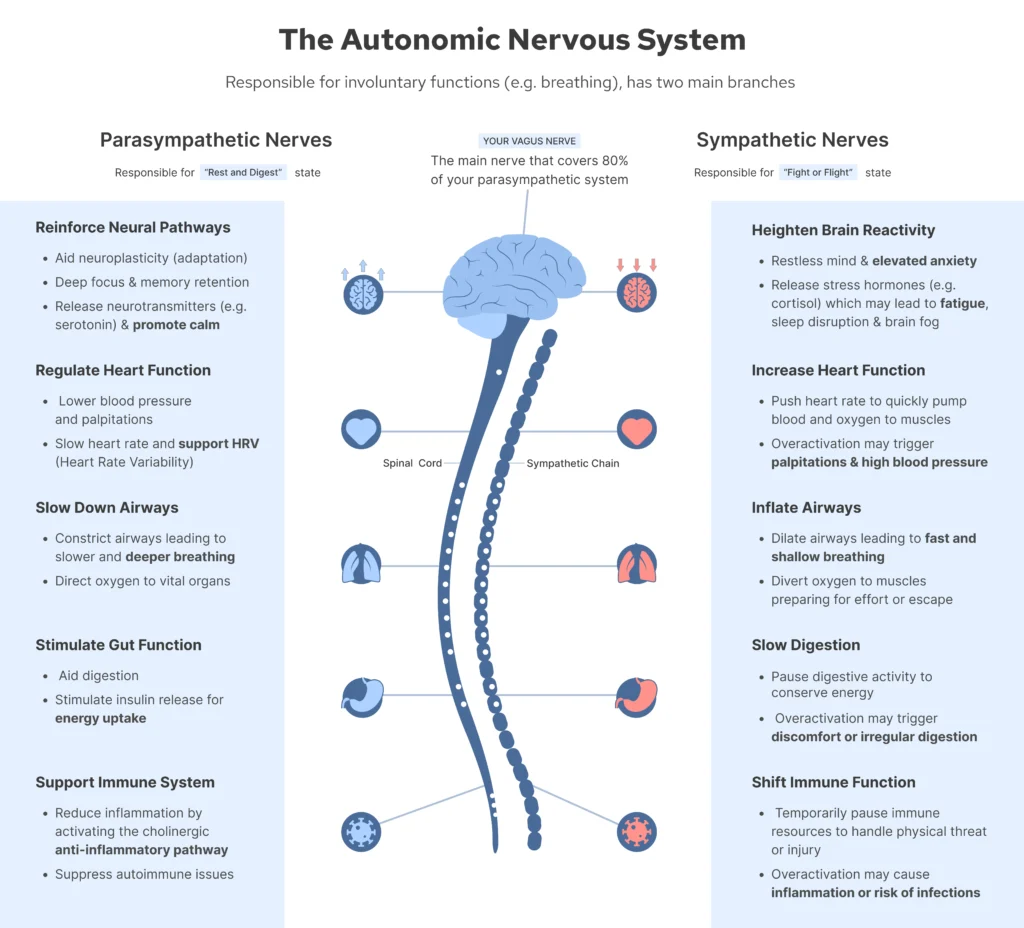
The Two-Mode System
Your autonomic nervous system operates through two complementary divisions:
- Increases heart rate, elevates cortisol, suppresses digestion, and mobilises energy reserves. Essential for short-term survival and acute stress response.
- Controlled predominantly by the vagus nerve, it reduces heart rate, promotes cellular repair, facilitates deep sleep, restores immune function, and replenishes energy reserves.
Genuine recovery (the kind that restores energy at the cellular level) can occur only in the parasympathetic state. When the vagus nerve is functioning well, your body shifts fluidly between these two modes.
You respond to stress and then fully recover.
But when vagal tone is impaired, the nervous system can become locked in a chronic low-grade sympathetic state:
– Burning energy reserves continuously
– Blocking restorative sleep
– Sustaining inflammation
– Making tiredness a structural feature of daily life rather than a passing symptom.
How Vagus Nerve Dysfunction Causes Tiredness
When your vagus nerve demonstrates reduced activity (low vagal tone):
- The parasympathetic nervous system drives mitochondrial energy production. Without adequate vagal tone, the body cannot fully activate the metabolic pathways responsible for producing ATP, the fundamental unit of cellular energy. The result is tiredness that originates at the cellular level, not simply at the level of motivation or effort.
- A poorly functioning vagus nerve loses its capacity to apply the brakes to the sympathetic nervous system. The body remains in a low-grade fight-or-flight state around the clock, burning through energy reserves, elevating cortisol, suppressing recovery hormones, and maintaining a state of physiological alertness that is profoundly exhausting over time.
- The vagus nerve plays a direct role in regulating sleep architecture, particularly slow-wave and REM sleep, the stages responsible for physical repair and cognitive restoration. Low vagal tone disrupts sleep at a structural level, producing nights that feel long but leave the body no more restored than before.
- The vagus nerve controls the cholinergic anti-inflammatory pathway. When it is impaired, the body cannot adequately suppress pro-inflammatory cytokines (TNF-α, IL-1β, IL-6). Elevated cytokine levels are directly associated with the subjective experience of tiredness, brain fog, and malaise, a mechanism documented in symptoms ranging from post-viral tiredness to autoimmune disease.
- HRV is a validated biomarker of both vagal tone and recovery capacity. Individuals with chronic tiredness consistently demonstrate markedly reduced HRV. This reflects a nervous system that remains in a high-demand state and is unable to self-regulate toward rest and restoration.
- Approximately 80% of vagal fibres carry signals from the gut to the brain. When this communication is impaired, the body's capacity to regulate digestion, absorb nutrients efficiently, and manage gut-derived inflammation is compromised. All of this contributes directly to systemic tiredness and reduced energy availability.
It is important to note that chronic tiredness is a heterogeneous symptom. Vagus nerve dysfunction does not account for all cases.
Some individuals exhibit predominant mitochondrial dysfunction; others, hormonal or nutritional deficiencies; and many demonstrate overlapping mechanisms.
Vagal impairment appears most relevant in individuals with reduced HRV, post-viral onset, inflammatory markers, or a pattern of tiredness that worsens with stress and improves with genuine rest.
The Scientific Evidence
Published research establishes clear relationships between vagus nerve dysfunction and chronic tiredness pathophysiology:
- Studies consistently document that individuals with Chronic Tiredness and persistent post-viral tiredness exhibit measurable autonomic abnormalities, including significantly reduced HRV, heightened sympathetic tone, and impaired parasympathetic recovery responses.
These autonomic signatures persist even when conventional tiredness markers (thyroid function, iron levels, and inflammatory panels) appear normal, suggesting a nervous-system origin that standard testing fails to capture.
- Research has established that elevated levels of pro-inflammatory cytokines (particularly IL-6, TNF-α, and IL-1β) directly induce tiredness, brain fog, and reduced motivation through their actions on the central nervous system.
The vagus nerve’s cholinergic anti-inflammatory pathway is the body’s primary mechanism for regulating these cytokine levels.
When vagal tone is impaired, this regulatory pathway is compromised, and inflammatory tiredness becomes chronic. Studies in autoimmune-associated tiredness, including joint pain and inflammatory gut symptoms, demonstrate that reduced vagal tone predicts greater tiredness severity independently of disease activity.
- Research on SARS-CoV-2 infection has identified vagal impairment as a key feature of Post-Viral Tiredness, with persistent tiredness among its most disabling manifestations.
Studies show that individuals with Post-Viral Tiredness exhibit significantly impaired vagal tone compared with those who have fully recovered, and that autonomic rehabilitation targeting the vagus nerve yields measurable improvements in energy, cognitive function, and exercise tolerance.
A 2022 study published in EClinicalMedicine (The Lancet) found that transcutaneous VNS significantly improved tiredness scores and functional status in a Post-Viral Tiredness cohort, with users reporting sustained improvements after 8 weeks of daily stimulation.
- Research consistently demonstrates that baseline HRV predicts tiredness severity, recovery capacity, and response to physical and psychological demands.
Multiple studies show that interventions that increase HRV (including VNS) produce corresponding improvements in subjective tiredness, cognitive performance, and physical stamina.
Here is why this matters:
Studies using Nuropod’s AVNT™ technology have documented a 61% improvement in vagal tone metrics, directly addressing the autonomic signature that underlies tiredness in dysregulated nervous system states.
- Peer-reviewed studies demonstrate that vagus nerve stimulation improves sleep quality by directly modulating sleep-stage regulation, reducing sympathetic arousal during sleep and increasing the proportion of slow-wave sleep, which is associated with physical recovery.
Given the central role of non-restorative sleep in perpetuating chronic tiredness, this represents a mechanistically relevant pathway for energy restoration beyond simple symptom management.

The mechanistic conclusion is simple:
Restoring vagus nerve function through targeted stimulation addresses the underlying autonomic, inflammatory, and metabolic pathophysiology of chronic tiredness (including sympathetic overdrive, neuroinflammation, sleep disruption, and impaired cellular energy production) rather than merely managing tiredness at a surface level.
VNS Devices as a Solution: How They Work
The Technology Revolution
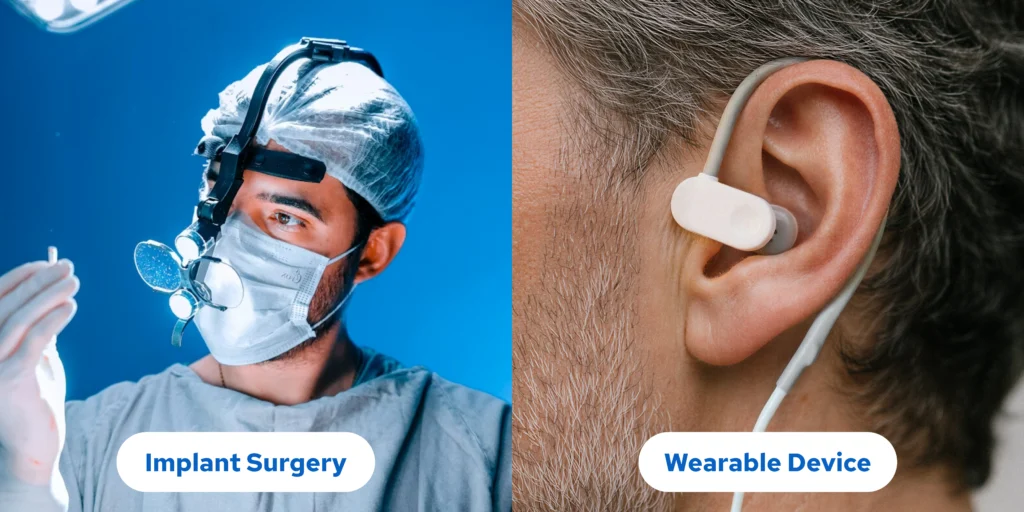
Until recently, vagus nerve stimulation required invasive surgical procedures, implanting electrodes directly on the nerve through operations that may carry hazards, extended recovery periods, and permanent device placement.
This confined VNS therapy primarily to therapy-resistant cases of depressive states and neurological issues, where the severity of the symptoms justified a surgical approach.
Today’s breakthrough changes everything.
Modern transcutaneous vagus nerve stimulation (tVNS) delivers the same therapeutic electrical impulses to the vagus nerve (facilitating neuroplastic adaptation and genuine restoration of autonomic tone) completely non-invasively through the skin.
– No surgery
– No implantation
– No recovery period is required
These advanced wearable devices achieve scientifically meaningful effectiveness with an exceptional safety profile, operating through precisely positioned electrodes at two accessible locations:
- Targeting the cervical branch of the vagus nerve near the carotid artery, where the nerve runs close to the skin's surface.
- Targeting the auricular branch of the vagus nerve at the tragus, the only location where cranial nerves reach the body's surface, offering direct and precise access.
This represents a fundamental shift.
Vagus nerve stimulation therapy that was once confined to operating rooms is now available for daily home use, with scientific-grade precision and zero surgical risk.
Mechanism of Action
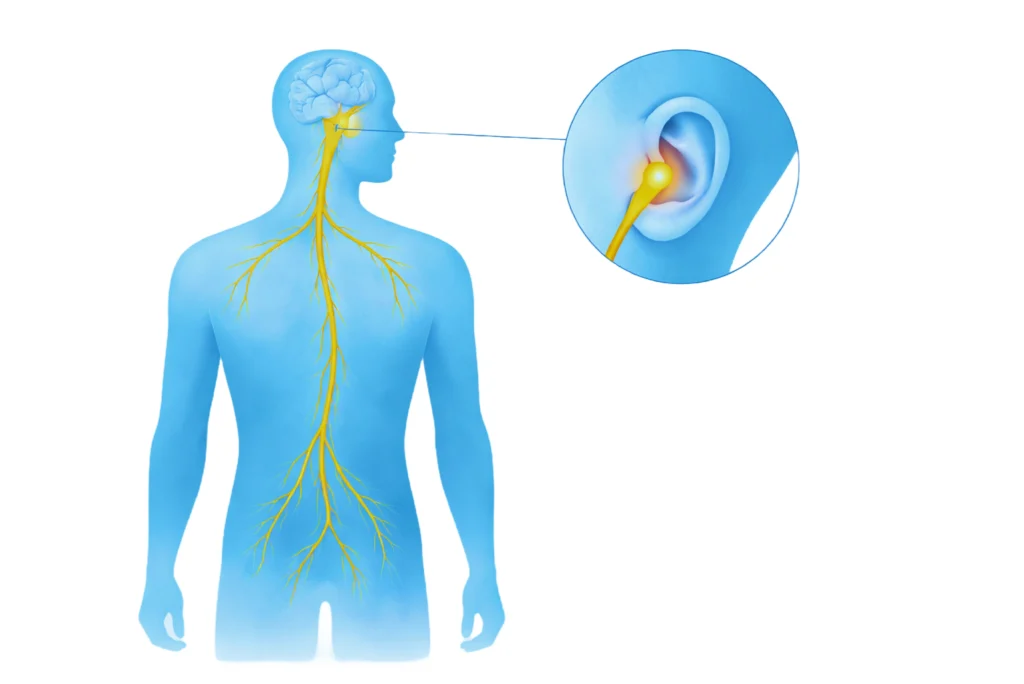
When precisely calibrated electrical impulses reach the vagus nerve, they initiate a cascade of neurophysiological responses:
- Stimulation triggers the release of acetylcholine at parasympathetic terminals, directly counteracting sympathetic dominance and activating the cholinergic anti-inflammatory pathway, suppressing the cytokines that drive inflammatory tiredness.
- Afferent vagal signals project to the nucleus tractus solitarius, which integrates autonomic regulatory information and modulates both cardiovascular control centres and sleep-wake circuitry in the medulla.
- Consistent stimulation protocols facilitate a measurable shift from sympathetic dominance towards parasympathetic restoration, improving HRV, lowering resting heart rate, and creating the physiological symptoms in which genuine recovery becomes possible.
- Parasympathetic activation supports mitochondrial energy production through improved metabolic regulation and oxidative phosphorylation. As the nervous system shifts out of chronic fight-or-flight, cellular energy production improves at a biochemical level.
- VNS suppresses sympathetic arousal during sleep, increases slow-wave sleep proportion, and supports the circadian signalling that governs restorative sleep, allowing the body to recover in the way that sleep is biologically designed to provide.
Scientific Parameters
Research-validated VNS protocols for tiredness typically employ:
- 30 to 60 minutes daily, allowing for sustained neurophysiological effects and cumulative autonomic adaptation.
- Individualised to sensory threshold, perceptible but comfortable stimulation. Strong enough to be felt, gentle enough to sustain without discomfort.
- Daily application for a minimum of 8 to 12 weeks. Neuroplastic change and genuine autonomic recalibration require time. The goal is restoration, not temporary relief.
Expected Timeline
VNS promotes gradual nervous system adaptation rather than immediate symptom suppression:
- Enhanced relaxation during and after stimulation sessions. Modest improvements in sleep quality reported by most users. Slight reduction in the wired-but-tired sensation. Early signs of improved HRV on wearable trackers.
- Noticeable improvements in morning energy. Reduced post-exertional crash duration and severity. Improved cognitive clarity during peak hours. Less reliance on caffeine to maintain baseline function.
- Sustained energy improvements across the day. Better sleep quality with measurably longer periods of restorative sleep. Reduced inflammatory tiredness responses. Improved exercise tolerance and reduced recovery time after activity.
- Restored autonomic balance supporting consistent daily energy. Functional capacity improvements allow re-engagement with work, social activity, and exercise. Measurable HRV gains reflecting genuine nervous system recalibration. Reduced dependence on tiredness management strategies.
Safety Considerations
VNS via transcutaneous approaches is generally well tolerated in scientific research. Potential transient responses may include:
- Mild tingling sensation at the stimulation site during use
- Temporary muscle tension in the neck region with cervical devices
- Brief lightheadedness in the initial sessions, typically resolving with protocol adjustment
Important limitations: Not appropriate for individuals with cardiac pacemakers, recent acute cardiac events, pregnancy, or a history of vagotomy.
Health professional consultation is essential before initiating any VNS protocol, particularly for individuals managing complex or multisystem symptoms.
Tiredness in Postural Heart Rate Abnormalities

Postural Heart Rate Abnormalities is a symptom of autonomic nervous system dysfunction affecting an estimated 1 to 3 million people in the United States.
And it goes even further:
One of its most debilitating yet least discussed features is profound, persistent tiredness, tiredness that does not correlate with sleep duration or activity level.
In Postural Heart Rate Abnormalities, the autonomic nervous system is unable to manage the cardiovascular demands of simply standing upright.
The heart accelerates to compensate, blood pools in the lower limbs, and the brain receives less oxygen.
The body enters a state of physiological alarm with every postural change and sustains it.
And the result?
It’s not just the dizziness and rapid heartbeat that define the symptom. It is exhaustion that accumulates with every hour spent awake and upright.
The vagal connection is direct.
Research documents markedly reduced HRV in individuals with Postural Heart Rate Abnormalities, reflecting parasympathetic withdrawal and an inability of the nervous system to self-regulate. Sympathetic overdrive (the body’s compensatory response to this withdrawal) is metabolically expensive. It depletes energy reserves rapidly and prevents the rest-and-digest recovery that replenishes them.
This study proved it:
A randomised, double-blind, placebo-controlled scientific study conducted at the University of Oklahoma Health Sciences Center demonstrated that auricular vagus nerve stimulation produced a scientifically meaningful reduction in postural rapid heartbeat –
- From 32±14 bpm in the placebo group
- To 18±10 bpm in the active group (p=0.016)
– alongside a significant reduction in anti-autonomic autoantibodies.
For individuals whose tiredness is driven by the constant cardiovascular strain of Postural Heart Rate Abnormalities, addressing the underlying vagal dysfunction is a mechanistically sound and scientifically supported approach.
Tiredness and Post-Viral Tiredness

For millions of people worldwide, persistent tiredness did not arrive gradually. It arrived after a viral illness, and it never left.
And the data is revealing:
Post-Viral Tiredness, most commonly associated with SARS-CoV-2 infection, is now one of the most prevalent and poorly understood sources of chronic tiredness globally.
Estimates suggest that between 10% and 30% of individuals who contract SARS-CoV-2 experience persistent symptoms beyond 12 weeks, with debilitating tiredness consistently reported as the most common and most functionally disabling.
The vagus nerve is a central player in this picture.
Research has documented direct vagal nerve damage following SARS-CoV-2 infection, with the virus demonstrating the capacity to access the autonomic nervous system via the ear, the precise anatomical site targeted by auricular VNS.
Even worse…
Studies consistently show that individuals with Post-Viral Tiredness exhibit profoundly impaired vagal tone compared to those who have fully recovered, alongside elevated inflammatory cytokines, disrupted HRV, and a nervous system locked in a sympathetic-dominant state that resists all conventional recovery approaches.
This is why standard tiredness management advice (pacing, rest, graduated exercise) provides incomplete relief for so many people with Post-Viral Tiredness.
It addresses behaviour, it does not address the underlying nervous system dysfunction that makes recovery physiologically impossible.
And here’s why it matters:
A 2022 study published in EClinicalMedicine (The Lancet) demonstrated that transcutaneous VNS produced significant improvements in tiredness scores and functional capacity in a Post-Viral Tiredness cohort, with users reporting sustained benefit after 8 weeks of daily stimulation.
A further study published in Clinical Cardiology (2025) reported that vagus nerve stimulation attenuated symptoms of Postural Heart Rate Abnormalities in users following SARS-CoV-2 infection, suggesting a shared autonomic mechanism linking post-viral tiredness, Postural Heart Rate Abnormalities, and vagal impairment.
For individuals whose tiredness began with a virus, restoring vagal tone is not a complementary approach. It is a direct intervention against the mechanism that is maintaining the symptom.
Top 4 VNS Devices for Post-Viral Fatigue
#1: Nuropod

Price: 900 USD (Varies by region, with a 100 USD research subsidy available)
Type: Auricular (ear-worn)
Technology: AVNT by Parasym
Why #1:
- Supported by 50+ peer-reviewed publications from Harvard Medical School, UCLA, and leading research institutions worldwide. No other wearable VNS device comes close to this evidence base.
- Scientific studies document a 61% improvement in vagal tone (HRV metrics), a significant reduction in sympathetic overactivation, improved sleep architecture, and reduced inflammatory markers. All of these are directly implicated in the pathophysiology of chronic tiredness. Demonstrated efficacy for autonomic dysregulation and tiredness.
- CE-marked as a wearable device meeting rigorous safety and performance standards, verified by an independent third-party assessment.
- Used by 1,000+ health professionals and researchers and integrated into institutional protocols. More than 4,000,000 supervised stimulation user sessions completed.
- Protocols derived from peer-reviewed research, not marketing assumptions. Placement at the tragus of the ear (as used in scientific studies on vagus nerve stimulation) is the safest and most precise method for achieving vagal access without surgery.
- 30-day evaluation period, science-based guidance resources, and responsive technical support from a team grounded in scientific research.
Best for:
Individuals experiencing persistent tiredness are seeking the most scientifically validated wearable device available, particularly those with Post-Viral Tiredness, Postural Heart Rate Abnormalities, autonomic dysregulation, or who have tried conventional solutions without adequate results.
#2: Truvaga Plus

Price: $544+ (Device $499 + conductive spray $45/year + potential subscription)
Type: Cervical (neck-held, handheld)
Shares core technology with gammaCore, an FDA-cleared device for headache and cluster headache. Delivers rapid parasympathetic effects and follows a straightforward protocol for users who prefer cervical stimulation.
Considerations:
- Ongoing costs for conductive spray, plus potential app subscription fees, add up; verify the total annual price before purchase.
- Known adverse effects include muscle spasms, facial droop, lip pull, and localised headache in a subset of users.
- Not suitable for individuals with cardiac symptoms, pacemakers, or recent cardiovascular events.
- Multiple users report mobile app connectivity issues.
- FDA clearance is for headache, not for tiredness or autonomic dysfunction.
Best for: Those who prefer cervical stimulation with an FDA-cleared technology lineage and can tolerate the potential for facial muscle spasm adverse effects.
#3: Pulsetto

Price: $350–$371 (Device $269 + conductive gel $81–$102/year)
Type: Cervical (hands-free collar)
Offers a hands-free wearable design, HSA/FSA eligibility, and a 2-year warranty. A lower entry price makes it appear more accessible.
Critical limitations:
- No scientific studies demonstrating efficacy for tiredness, autonomic dysregulation, or any chronic symptom, only company press releases and retail testimonials.
- Frequent fit problems lead to inadequate nerve contact, particularly for individuals with smaller necks, thereby compromising therapeutic delivery at a structural level.
- Users managing tiredness consistently report minimal to no measurable improvement compared to research-validated devices.
Not recommended for chronic tiredness: The £200 to £300 price difference appears attractive until you consider the real cost, months of continued exhaustion while using an unproven device. When tiredness is already limiting your capacity to work, function, and live fully, the absence of scientific validation is not a minor consideration.
#4: Sensate

Price: $299–$349
Type: Chest-worn vibrotactile device (not true VNS)
A comfortable pebble-shaped device worn on the chest. Simple app interface with accompanying soundscapes. Lower price point. It can be used whilst resting or lying down.
Critical distinction:
- Sensate does not stimulate the vagus nerve through electrical impulses. It uses infrasonic vibrations and bone conduction applied to the sternum, an indirect approach that targets general relaxation rather than specific activation of the vagal nerve.
- Actual vagus nerve stimulation devices deliver calibrated electrical signals directly to accessible vagal branches. Sensate delivers vibrations to the chest, hoping for downstream effects.
For individuals with chronic tiredness or Post-Viral Tiredness:
This distinction matters significantly. Tiredness driven by autonomic dysregulation requires restoration of measurable nervous system function, improved HRV, suppression of inflammatory cytokines, restoration of sleep architecture, and recalibration of the sympathetic-parasympathetic balance.
A general relaxation device may reduce momentary stress, but does not address the underlying vagal dysfunction that prevents the body from recovering energy at a physiological level.
No scientific studies demonstrate Sensate’s efficacy for tiredness, autonomic symptoms, or Post-Viral Tiredness; only company-funded studies have shown mild stress reduction in healthy volunteers.
Best for: Those seeking a general relaxation and wind-down tool rather than targeted vagus nerve stimulation for tiredness and autonomic recovery.
Not recommended for individuals prioritising evidence-based tiredness therapy.
Conclusion: Nuroppod offers the most comprehensive scientific validation, proven efficacy for the autonomic dysregulation that drives chronic tiredness (including its manifestations in Postural Heart Rate Abnormalities and Post-Viral Tiredness), independent regulatory certification, and the strongest evidence base for individuals ready to address the root cause of their exhaustion rather than manage it indefinitely.
Take Action
Persistent tiredness driven by vagus nerve dysfunction and autonomic dysregulation is not a character flaw, a lifestyle problem, or an inevitable part of getting older.
Your autonomic nervous system possesses the capacity for neuroplastic adaptation and genuine restoration of regulatory function, given the right support.
With backing from 50+ scientific studies, independent CE-marking certification, and more than 4,000,000 documented stimulation sessions worldwide, Nuropod provides the most scientifically validated approach available for restoring autonomic balance, improving cellular energy, and recovering the functional capacity that tiredness has taken from you.
This blog post aims to be informational and should not replace professional health advice. Always consult with a health professional for personalised advice.
Sources
- Bonaz B, Bazin T, Pellissier S. The Vagus Nerve at the Interface of the Microbiota-Gut-Brain Axis. Frontiers in Neuroscience. 2018;12:49.
- Stavrakis S, Chakraborty P, Farhat K, et al. Noninvasive Vagus Nerve Stimulation in Postural Tachycardia Syndrome. JACC: Scientific Electrophysiology. 2023 Nov 1.
- Wang Z, Zhu T, Li X, Lai X, Chen M. Tragus Nerve Stimulation Attenuates Postural Orthostatic Tachycardia Syndrome in Post COVID-19 Infection. Clinical Cardiology. 2025 Feb 27;48(3).
- Breit S, Kupferberg A, Rogler G, Hasler G. Vagus Nerve as Modulator of the Brain-Gut Axis in Psychiatric and Inflammatory Disorders. Frontiers in Psychiatry. 2018;9:44.
- Tracey KJ. The inflammatory reflex. Nature. 2002;420(6917):853–859.
- Thayer JF, Åhs F, Fredrikson M, Sollers JJ, Wager TD. A meta-analysis of heart rate variability and neuroimaging studies: implications for heart rate variability as a marker of stress and health. Neuroscience & Biobehavioural Reviews. 2012;36(2):747–756.
- Komaroff AL, Lipkin WI. Insights from myalgic encephalomyelitis/chronic tiredness may help unravel the pathogenesis of post-acute COVID-19 syndrome. Trends in Molecular Medicine. 2021;27(9):895–906.
Share via:

