A comprehensive review of how VNS devices enhance cardiovascular resilience by optimising autonomic nervous system balance, with expert rankings of the top 4 certified options.

Heart Rate Variability (HRV) has emerged as one of the most powerful biomarkers of health, stress resilience, and longevity. Unlike your resting heart rate (which simply tells you how many times your heart beats per minute), HRV measures something more revealing: the beat-to-beat fluctuations in the timing between consecutive heartbeats.
Recent cardiovascular research demonstrates that higher HRV is associated with better stress resilience, improved recovery capacity, better cardiovascular fitness, and a reduced risk of future health complications, including cardiac events and all-cause mortality. Individuals with chronically low HRV are associated with elevated health risks, often reflecting chronic stress exposure, reduced physiological adaptability, and markers of accelerated biological ageing.
This guide examines the relationship between HRV and autonomic nervous system function. It evaluates the leading vagus nerve stimulation (VNS) devices that may help optimise HRV and enhance overall health resilience.
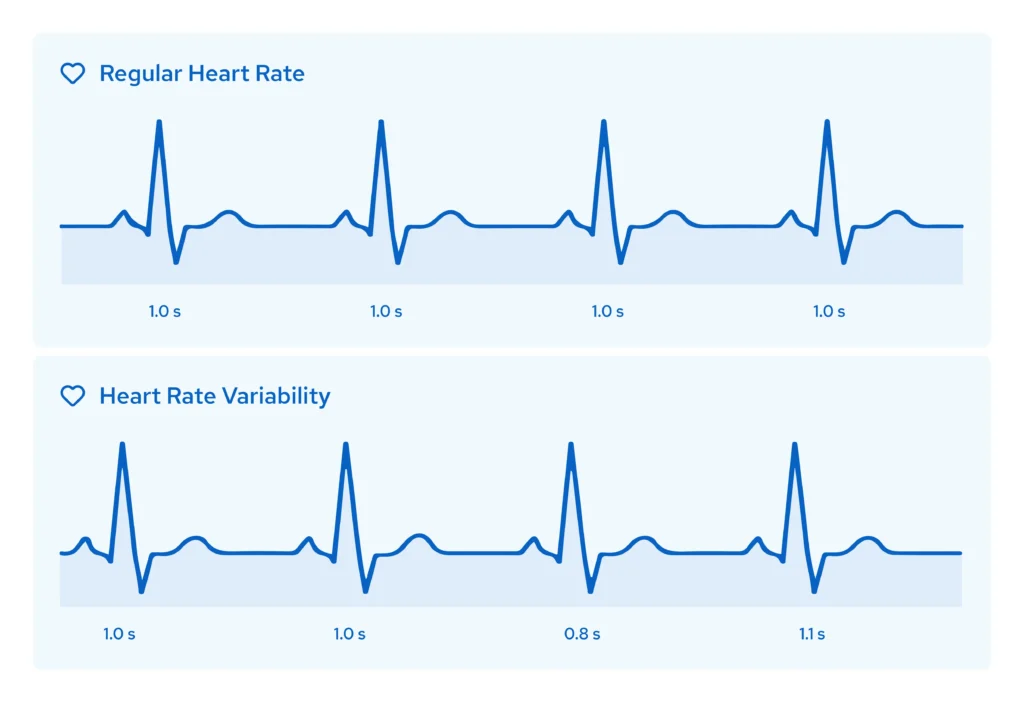
Understanding Heart Rate Variability
Heart Rate Variability refers to the natural fluctuation in the time interval between consecutive heartbeats. Even when your heart rate remains steady at 60 beats per minute, the exact interval between beats varies: one beat might occur 0.8 seconds after the last, the next 1.0 seconds later. These micro-variations, measured in milliseconds, are imperceptible without specialised devices yet reveal critical information about the autonomic nervous system.
Key HRV metrics include:
Time-domain measurements:
- SDNN (Standard Deviation of NN intervals): Reflects overall HRV and autonomic nervous system activity
- RMSSD (Root Mean Square of Successive Differences): Indicates short-term vagal-mediated HRV
- pNN50 (Percentage of successive intervals differing by >50ms): Measures parasympathetic activity
Frequency-domain measurements:
- High-Frequency (HF) power: Reflects parasympathetic (vagal) activity
- Low-Frequency (LF) power: Reflects both sympathetic and parasympathetic influences
- LF/HF ratio: Indicates autonomic balance
What do HRV numbers indicate?
- High HRV: Generally indicates a healthy, adaptable cardiovascular system with balanced parasympathetic activity. Reflects the body's ability to readily adjust to changes and stressors. Associated with lower stress levels and greater resilience.
- Low HRV: Often a warning sign of reduced adaptability. The body remains in a stressed, or "fight-or-flight," state, with slight variation between beats. Scientifically linked to current or future health problems, indicating an overactive stress response or compromised recovery capacity.
Higher HRV (in the absence of arrhythmias) correlates with better cardiovascular fitness, stress resilience, and nervous system balance, whereas low HRV signals stress, tiredness, or underlying health issues.
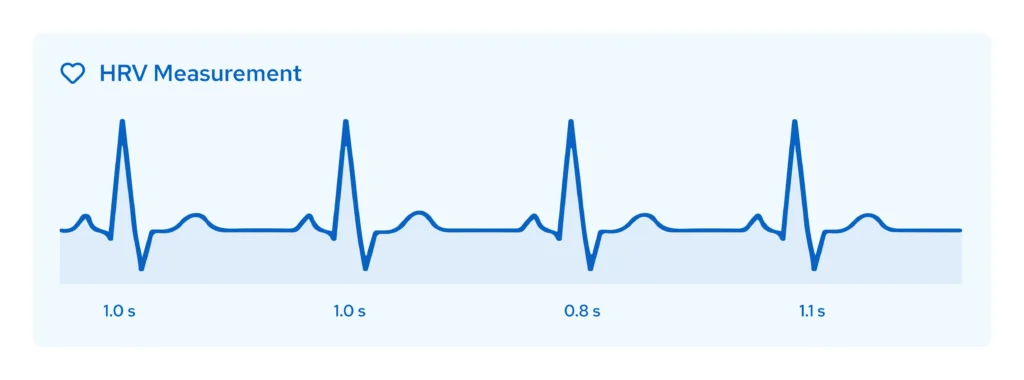
HRV Self-Assessment
Evaluate the factors that may be affecting your HRV:
Stress & Recovery Indicators
- Experience chronic work or life stress
- Poor stress management strategies
- Difficulty "switching off" after stressful events
- Racing thoughts or rumination
- Tension headaches or muscle tightness
Sleep Quality
- Frequently wake during the night
- Sleep less than 7 hours regularly
- Wake feeling unrefreshed despite adequate sleep time
- Shift work or irregular sleep schedule
- Sleep disrupted by stress or anxious thoughts
Cardiovascular & Fitness
- Sedentary lifestyle with minimal aerobic exercise
- Cardiovascular disease or hypertension
- Blood sugar regulation problems or metabolic syndrome
- Overtraining symptoms (persistent tiredness, declining performance)
- Extended recovery periods after exercise
Lifestyle Factors
- Regular alcohol consumption (especially evening drinking)
- Poor hydration habits
- Irregular meal timing or late-night eating
- High caffeine consumption
- Chronic inflammatory symptoms
Health Status
- Frequent illness or infections
- Chronic pain symptoms
- Autoimmune disorders
- Depressive states or anxious thoughts
- Age-related decline in cardiovascular function
HRV Tracking Experience
- Wearable device shows consistently low HRV values
- HRV declining over time despite no obvious changes
- Large day-to-day HRV fluctuations
- HRV drops sharply before illness symptoms appear
- HRV remains suppressed for days after stress or exercise
If you identify with multiple factors across stress, sleep, and cardiovascular categories, your HRV may be suboptimal. Low HRV isn’t merely a number; it reflects reduced autonomic flexibility and potentially compromised health resilience.
Vagus nerve stimulation may warrant consideration as a non-pharmacological approach to optimising autonomic balance and enhancing HRV.
The Vagus Nerve Connection
What Is the Vagus Nerve?
The vagus nerve (cranial nerve X) is the longest and most complex nerve of the autonomic nervous system. It originates in the medulla oblongata and projects through the neck to innervate the heart, lungs, and gastrointestinal tract. It mediates critical homeostatic functions:
- Cardiovascular regulation (heart rate modulation)
- Respiratory pattern generation
- Gastrointestinal motility and secretion
- Inflammatory reflex pathway (cholinergic anti-inflammatory response)
- Baroreceptor reflex integration
- Stress response modulation
Crucially, the vagus nerve is the primary parasympathetic nerve influencing the heart. It acts as a brake on the heart, slowing the sinoatrial node pacemaker and allowing more variability between beats. HRV is widely regarded as a non-invasive biomarker of vagal tone (parasympathetic activity) in the body.
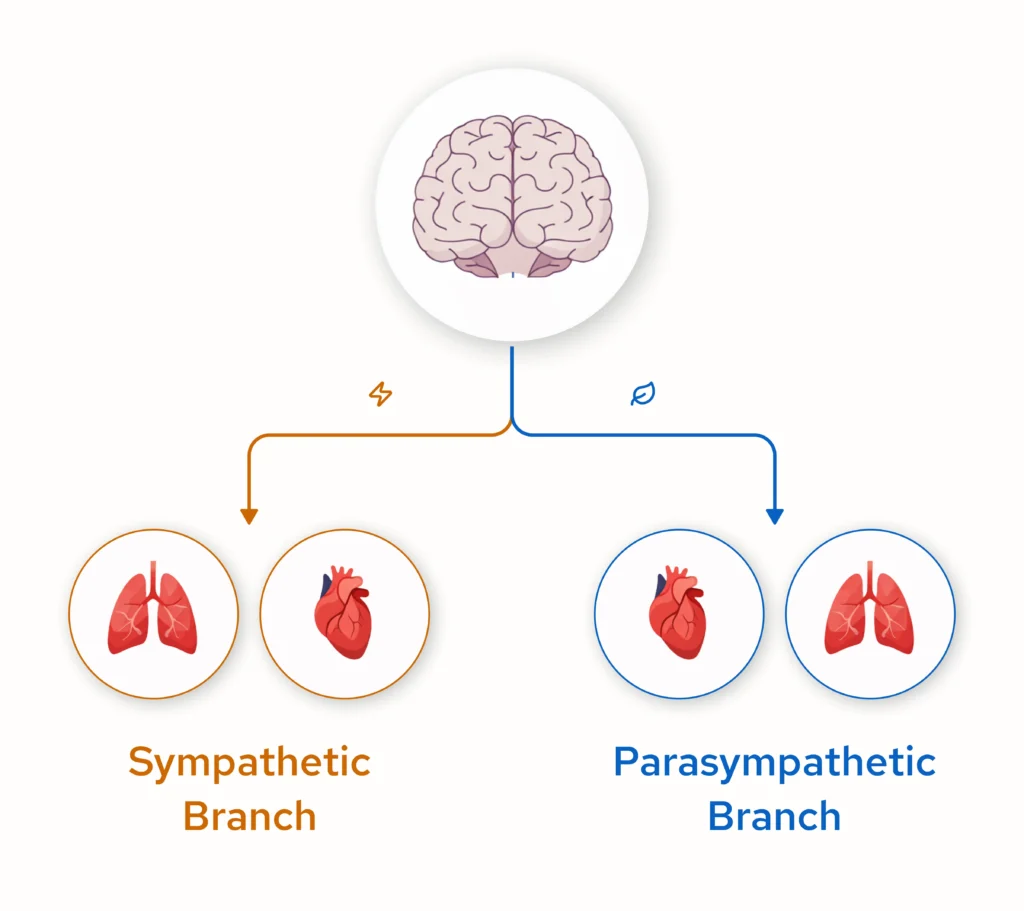
The Two-Mode System
Your autonomic nervous system operates through two complementary divisions:
- Sympathetic nervous system (SNS): Increases heart rate, elevates blood pressure, mobilises glucose, and prepares the body for action. It is activated during stress, exercise, or perceived threat. Creates more regular heartbeats (low variability).
- Parasympathetic nervous system (PNS): Controlled predominantly by the vagus nerve, reduces heart rate, promotes digestion and recovery, supports cellular restoration. Creates more variable heartbeats (high variability).
Healthy autonomic function requires a dynamic balance among these systems, with rapid shifts in response to environmental demands and metabolic needs. When vagal tone is high, the heart can rapidly adjust from moment to moment, producing higher variability. When vagal activity is low, HRV drops as the heart maintains a more locked, rapid rhythm.
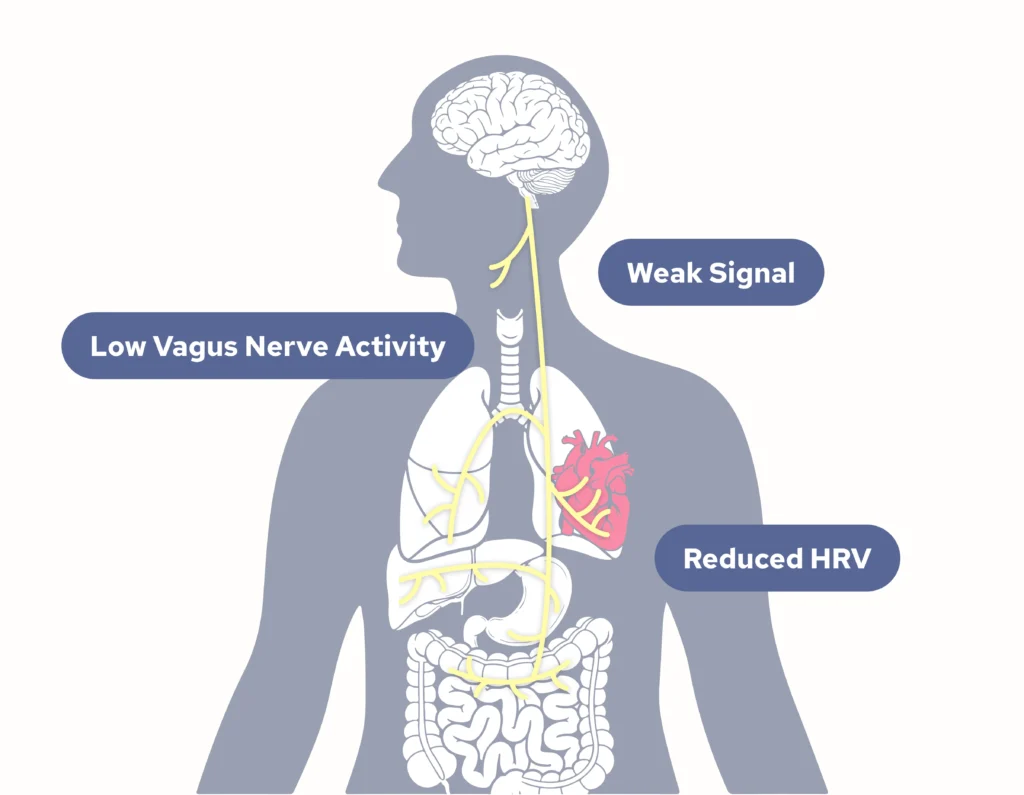
How Low Vagal Tone Reduces HRV
When your vagus nerve demonstrates reduced activity (low vagal tone), multiple physiological consequences reduce HRV:
- Loss of Parasympathetic Influence: Without adequate vagal "braking," the heart remains under sympathetic dominance, beating rapidly and regularly with minimal variation. The push-pull dynamic between SNS and PNS, which creates healthy variability, diminishes.
- Chronic Stress State: Persistently elevated stress hormones (cortisol, norepinephrine) maintain the body in fight-or-flight mode. The sympathetic nervous system stays activated, suppressing the vagus nerve's calming influence and drastically reducing beat-to-beat variability.
- Reduced Respiratory Sinus Arrhythmia: The normal, healthy increase in heart rate during inhalation and decrease during exhalation (respiratory sinus arrhythmia) is a vagally-mediated phenomenon. Low vagal tone diminishes this natural rhythm, resulting in a more monotonous heart rate pattern.
- Impaired Recovery Capacity: The vagus nerve facilitates physiological recovery after stress or exertion. When vagal activity is compromised, recovery takes longer, and HRV remains suppressed. This manifests as prolonged elevated heart rate after exercise, poor overnight HRV recovery, and persistent tiredness.
- Inflammatory Dysregulation: The vagus nerve controls the cholinergic anti-inflammatory pathway. Dysfunction permits chronic low-grade inflammation, which directly impairs cardiovascular function and further suppresses HRV. Inflammatory cytokines interfere with autonomic nervous system signalling.
- Reduced Baroreceptor Sensitivity: The vagus nerve transmits arterial baroreceptor signals to the brainstem. Dysfunction impairs this feedback loop, preventing appropriate cardiovascular adjustments and reducing the moment-to-moment variability that reflects healthy autonomic responsiveness.
- Accelerated Biological Ageing: Age-related HRV decline is partially mediated by progressive loss of vagal tone. However, chronically low vagal activity at any age accelerates this process, essentially ageing your cardiovascular system prematurely.
The critical insight: HRV is not merely a passive measurement of heart function; it reflects, in part, vagal nerve activity and overall autonomic regulation. Restoring vagal tone through targeted interventions can meaningfully elevate HRV and the health benefits it represents.

The Scientific Evidence
Published research establishes clear relationships between vagus nerve activity and HRV:
- HRV as a Vagal Biomarker: Decades of autonomic nervous system research confirm that HRV (particularly time-domain metrics such as RMSSD and frequency-domain high-frequency power) is a validated, non-invasive biomarker of cardiac vagal tone. When vagal activity increases, HRV rises proportionally. When vagal activity declines, HRV drops correspondingly.
- HRV and Health Outcomes: Dozens of longitudinal studies across diverse populations show that low HRV is a strong, independent predictor of adverse health outcomes. Individuals with very low HRV face a significantly higher risk of heart attacks, cardiac arrhythmias, stroke, and all-cause mortality. Conversely, people with exceptionally long life spans (healthy centenarians) tend to have relatively well-preserved HRV for their age.
- HRV and Stress Resilience: Research shows that higher HRV correlates with better stress tolerance, emotional regulation, and cognitive performance. Studies confirm that optimal vagally-mediated HRV is associated with efficient executive function and emotional stability. Individuals with higher HRV report feeling less stressed and more emotionally balanced in daily life.
- HRV Decline with Chronic Stress: Scientific studies document that chronic psychological stress, physical overtraining, sleep deprivation, and inflammatory symptoms all suppress HRV through mechanisms involving vagal withdrawal and sympathetic predominance. Alcohol consumption, poor nutrition, and illness reliably decrease overnight HRV measurements.
- Scientific trial evidence for vagus nerve stimulation: Multiple randomised controlled studies demonstrate that transcutaneous vagus nerve stimulation (tVNS) significantly increases HRV metrics compared to sham stimulation:
- Geng et al. (2022) - Randomised Study: Transcutaneous auricular VNS (taVNS) significantly increased multiple HRV measures in healthy young adults compared to sham stimulation. Metrics including RMSSD, pNN50, SDNN, and high-frequency power all increased during active VNS relative to baseline. Notably, some HRV improvements persisted even after stimulation ended, with HF power and pNN50 remaining elevated during post-stimulation recovery, suggesting lasting parasympathetic enhancement.
- Dose-Dependent Effects: Research demonstrates that appropriately tuned VNS parameters yield greater HRV enhancement. Targeting nerve-rich auricular regions (cymba conchae, inner tragus) with optimised electrical parameters produces a notable increase in HRV in healthy volunteers.
- Scientific Populations: Studies on individuals with autonomic dysfunction (including Postural Heart Rate Abnormalities, heart problems, and post-viral syndromes) found that regular daily VNS increases HRV over weeks of therapy, correlating with symptom improvements and enhanced functional capacity.
- Mechanism Confirmation: VNS triggers the release of acetylcholine at parasympathetic terminals and activates the cholinergic anti-inflammatory pathway. This shifts autonomic equilibrium toward parasympathetic dominance, as reflected by elevated HRV.
- The mechanistic conclusion: Restoring vagus nerve function through targeted stimulation addresses the fundamental autonomic physiology underlying HRV, directly enhancing vagal tone and parasympathetic activity rather than merely suppressing symptoms or artificially manipulating heart rate.
VNS Devices as a Solution: How They Work
The Technology Revolution
Until recently, vagus nerve stimulation required invasive surgical procedures (implanting electrodes directly on the nerve through operations that carried surgical risks), recovery time, and permanent device placement. This confined VNS management primarily to therapy-resistant depressive states, where benefits justified surgical intervention.
Today’s breakthrough changes everything.
Modern transcutaneous vagus nerve stimulation (tVNS) delivers the same therapeutic electrical impulses to the vagus nerve (facilitating neuroplastic adaptation and restoring appropriate tone). Still, it does so completely non-invasively through the skin.
No surgery, no implantation, no recovery period.
These advanced devices achieve remarkable effectiveness with an exceptional safety profile, operating through precisely positioned electrodes at two accessible locations:
- Auricular (ear): Targeting the auricular branch of the vagus nerve, which innervates the ear: the only place cranial nerves reach the body's surface
- Cervically (neck): Targeting the cervical branch of the vagus nerve near the carotid artery, where the nerve courses superficially beneath the skin. While the nerve does run close to the skin's surface here, this approach comes with limitations. The neck site stimulates indiscriminately (activating surrounding muscle tissue and nearby nerves alongside the vagus) making precise, controlled delivery difficult. Neck devices also require users to hold the device against the throat during each session, making hands-free use impractical. Critically, the cervical approach represents a far smaller body of clinical research, with far less scientific consensus on safety and long-term efficacy.
This represents a fundamental shift: vagus nerve stimulation therapy, once confined to operating rooms, is now available for daily home use with scientific-grade precision and zero surgical risk.
Mechanism of Action
When precisely calibrated electrical impulses reach the vagus nerve, they initiate a cascade of neurophysiological responses that enhance HRV:
- Direct Vagal Activation: Stimulation triggers afferent vagal signals that project to the nucleus tractus solitarius in the brainstem, where autonomic regulatory information is integrated, and cardiovascular control centres are modulated.
- Neurotransmitter Modulation: VNS triggers the release of acetylcholine at parasympathetic terminals, directly activating the vagal brake on the heart and increasing beat-to-beat variability.
- Autonomic Rebalancing: Consistent stimulation protocols facilitate a shift from sympathetic dominance toward parasympathetic restoration. This rebalancing is objectively measurable through HRV metrics: particularly increases in RMSSD, pNN50, and high-frequency power.
- Enhanced Respiratory Sinus Arrhythmia: VNS strengthens the vagal component of heart rate variability during breathing. During deep exhalation, enhanced vagus nerve activity produces greater heart rate deceleration, a hallmark of healthy HRV.
- Inflammatory Suppression: Vagal stimulation activates the cholinergic anti-inflammatory pathway, reducing pro-inflammatory cytokine production (TNF-α, IL-1β, IL-6) that suppresses HRV. Reduced inflammation improves cardiovascular autonomic function.
- Neuroplasticity Enhancement: Regular VNS promotes synaptic reorganisation in central autonomic networks, potentially restoring normal cardiovascular regulatory capacity and sustainably elevating baseline vagal tone.
Scientific Parameters
Research-validated VNS protocols for HRV optimisation typically employ:
- Session duration: 30-60 minutes daily (allowing for sustained neurophysiological effects)
- Intensity: Individualised to sensory threshold (perceptible but comfortable stimulation)
- Consistency: Daily application for a minimum of 4-8 weeks (neuroplastic changes and HRV improvements require sustained intervention)
- Timing: Often performed during relaxation or before sleep to maximise parasympathetic activation
Expected Timeline for HRV Improvement
VNS promotes gradual autonomic nervous system adaptation rather than immediate changes:
- Week 1-2: Enhanced relaxation response during stimulation sessions, improved sleep quality, and possible mild reduction in resting heart rate. Initial HRV improvements may be detectable during stimulation periods.
- Week 3-4: Noticeable improvements in stress tolerance, reduced resting heart rate, and better recovery from exercise. HRV metrics begin showing measurable increases on wearable devices. Enhanced sense of calm and emotional balance.
- Month 2-3: Sustained HRV elevation across multiple metrics (RMSSD, SDNN, HF power). Improved cardiovascular fitness markers, enhanced cognitive function, and reduced subjective stress levels. Many users report improved energy and reduced tiredness.
- Month 3+: Consolidated autonomic balance with stable, elevated HRV baseline. Enhanced stress resilience, optimised recovery capacity, improved overall health markers. Users often report feeling "younger" with better stress tolerance and physical resilience.
Important note: Individual responses vary based on baseline vagal tone, lifestyle factors, and adherence to protocols. Combining VNS with supportive lifestyle modifications (quality sleep, regular exercise, stress management, balanced nutrition) produces optimal results.
Safety Considerations
VNS using transcutaneous approaches has a strong safety profile in scientific research. Potential transient responses may include:
- Mild tingling sensation at the stimulation site
- Temporary muscle tension in the neck region (cervical devices)
- Brief lightheadedness (typically resolves with protocol adjustment)
- Skin irritation at electrode sites (rare, usually resolved with repositioning)
Important limitations: Not appropriate for individuals with implanted cardiac devices (pacemakers or defibrillators), recent acute cardiovascular events, pregnancy, history of vagotomy, or known cardiac arrhythmias without medical supervision. Consultation with a healthcare provider is essential before initiating any VNS protocol, particularly for those with cardiovascular symptoms.
VNS has an exceptionally favourable risk profile compared to pharmaceutical approaches for autonomic dysfunction, as it works with the body’s natural regulatory systems rather than overriding them.
Top 4 VNS Devices for HRV Optimisation
#1: Nuropod

Price: $900 ($100 research subsidy available)
Type: Auricular (ear-worn)
Technology: AVNT™ by Parasym
Why #1:
- Most extensively validated: Supported by 50+ completed scientific studies from 100+ elite research institutions like Yale, Stanford, Harvard, UCLA, University College London, Imperial College London, to name a few. The largest body of scientific evidence for any consumer VNS device.
- Demonstrated HRV improvements: Scientific studies document an average 61% improvement in vagal tone (HRV metrics), with significant increases in RMSSD, pNN50, SDNN, and high-frequency power. Users show measurable parasympathetic enhancement and reduced sympathetic overactivation.
- Independent certification: CE-marked device meeting rigorous safety and performance standards, third-party verified. Not merely a wellness gadget but a certified technology.
- Scientific adoption: Used and recommended by 1000+ licensed healthcare professionals; integrated into institutional protocols; 4,000,000+ happy user sessions completed.
- Evidence-based parameters: Stimulation protocols derived directly from peer-reviewed research, not proprietary guesswork or marketing claims.
- Long-term effectiveness: Research demonstrates sustained HRV improvements persist with regular use, indicating genuine neuroplastic changes rather than temporary effects.
- Comprehensive support: 30-day evaluation period, scientific guidance resources, and responsive technical support.
Best for: Individuals seeking the most scientifically validated device for HRV optimisation, particularly those prioritising evidence-based outcomes, long-term autonomic health, and proven effectiveness over marketing claims.
#2: Truvaga Plus

Price: $544+ (device $499 + spray $45/year + potential subscription)
Type: Cervical (neck handheld)
Technical note: Shares core technology with gammaCore, an FDA-cleared device for cluster headache prevention. Produces rapid parasympathetic effects with immediate heart rate reduction during stimulation.
Advantages: Strong acute HRV response during active stimulation. FDA-cleared technology lineage (though cleared for headache, not HRV optimisation specifically). Straightforward protocol requires minimal setup.
Considerations:
- Ongoing costs for conductive spray plus potential app subscription: verify total pricing before purchase
- Common adverse effects include neck muscle spasms, facial droop, lip pull, and headache
- Requires precise hand-held placement during each session: less convenient for longer sessions
- Not suitable for users with cardiac symptoms, pacemakers, or recent cardiovascular events
- Some users report mobile app connectivity problems
- Limited published research specifically demonstrating sustained HRV improvements (most studies focus on acute effects)
Best for: Those preferring cervical stimulation with FDA-cleared technology lineage who can tolerate potential facial muscle spasm adverse events and don’t mind hand-held operation during sessions.
#3: Pulsetto

Price: $350-$371 (device $269 + gel $81-$102/year)
Type: Cervical (hands-free collar)
Advantages: Hands-free wearable collar design, can be worn during other activities. Lower price point than Nuropod. HSA/FSA eligible. 2-year warranty coverage.
Critical Limitations:
- No peer-reviewed scientific studies demonstrating HRV improvements, only company press releases, proprietary white papers, and retail testimonials
- Frequent fit problems create inadequate nerve contact, especially with smaller necks, and users report inconsistent stimulation quality
- Collar design may not target optimal vagus nerve locations compared to research-validated ear or precise neck placement
- Users consistently report minimal to no measurable HRV improvements on wearable tracking devices compared to research-validated devices
- The absence of independent scientific validation means the effectiveness of HRV optimisation remains uncertain
Not recommended for serious HRV optimisation: The $200-350 price difference appears attractive until you calculate the real cost: weeks or months of daily use without measurable HRV improvement. For those prioritising evidence-based autonomic enhancement over general relaxation, devices with published research supporting their use provide greater confidence in outcomes.
May be suitable for: General stress reduction and relaxation support (rather than targeted HRV optimisation), users willing to accept uncertain outcomes, and those preferring hands-free convenience over proven effectiveness.
#4: Sensate

Price: $299-$349
Type: Chest-worn vibrotactile device (not true VNS)
Advantages: Comfortable pebble design worn on the chest. Simple app interface with soundscapes. Lower price point. It can be used while performing other activities with the neck strap. Pleasant user experience for relaxation.
Critical distinction:
Sensate does not directly stimulate the vagus nerve with electrical impulses, unlike other devices in this comparison. Instead, it uses infrasonic vibrations and bone conduction applied to the sternum, an indirect approach that targets general stress reduction rather than specific activation of the vagal nerve.
While bone conduction at specific auricular locations has research supporting vagal stimulation, Sensate’s chest placement lacks scientific evidence for directly engaging the vagus nerve. The mechanism is fundamentally different:
- Actual VNS devices (like Nuropod, Truvaga, and Pulsetto) deliver calibrated electrical signals directly to accessible vagus nerve branches, producing measurable vagal activation
- Sensate delivers vibrations to your sternum, hoping for downstream autonomic effects through indirect mechanisms
For HRV optimisation: This distinction matters profoundly. Optimising HRV requires restoring measurable vagal tone, as evidenced by demonstrable increases in RMSSD, pNN50, high-frequency power, and sustained parasympathetic activity. General relaxation devices may help with subjective stress perception but do not directly target the vagal mechanisms that elevate HRV.
Evidence gap: No published scientific studies demonstrate Sensate’s efficacy for HRV optimisation: only company-funded studies showing general stress reduction in healthy volunteers. No independent peer-reviewed research has validated HRV improvements comparable to those of true VNS devices.
Best for: Those seeking a general relaxation and meditation enhancement tool rather than targeted vagus nerve stimulation for HRV optimisation. Not recommended for individuals prioritising evidence-based autonomic nervous system enhancement and measurable HRV improvements.
Conclusion: Nuropod offers the most comprehensive scientific validation, proven efficacy for HRV enhancement, independent regulatory certification, and optimal balance of research foundation and practical application for those prioritising measurable autonomic nervous system optimisation.
Optimise Your HRV
Heart Rate Variability represents far more than a wearable device metric: it’s a window into your body’s adaptive capacity, stress resilience, and long-term health trajectory. Higher HRV correlates with reduced cardiovascular risk, enhanced stress tolerance, improved cognitive performance, and potentially extended healthspan.
Your autonomic nervous system possesses remarkable neuroplastic capacity. With targeted vagal stimulation, you can strengthen the parasympathetic “brake” on your heart, enhance beat-to-beat variability, and build the physiological resilience that characterises optimal health.
With support from 50+ completed scientific studies, independent CE-marking certification, and 4,000,000+ happy user sessions completed, Nuropod provides the most scientifically validated approach to enhancing vagal tone and optimising HRV.
Special Research Opportunity: Participate in ongoing HRV research and receive up to $100 off your Nuropod wellness product while contributing to the advancement of autonomic health science.
This information is provided for educational purposes. VNS devices are not intended to diagnose, treat, cure, or prevent any disease. Individuals with cardiovascular symptoms should work with qualified healthcare providers before beginning any VNS protocol. Always consult your physician before starting any new health intervention.
This blog post aims to be informational and should not replace professional health advice. Always consult with a health professional for personalised advice.
Sources
- Thayer JF, Yamamoto SS, Brosschot JF. The relationship of autonomic imbalance, heart rate variability and cardiovascular disease risk factors. International Journal of Cardiology. 2010;141(2):122-131.
- Laborde S, Mosley E, Thayer JF. Heart rate variability and cardiac vagal tone in psychophysiological research – recommendations for experiment planning, data analysis, and data reporting. Frontiers in Psychology. 2017;8:213.
- Tsuji H, Venditti FJ Jr, Manders ES, et al. Reduced heart rate variability and mortality risk in an elderly cohort. The Framingham Heart Study. Circulation. 1994;90(2):878-883.
- De Couck M, Caers R, Musch L, et al. How breathing can help you make better decisions: Two studies on the effects of breathing patterns on heart rate variability and decision-making in business cases. International Journal of Psychophysiology. 2019;139:1-9.
- Clancy JA, Mary DA, Witte KK, et al. Non-invasive vagus nerve stimulation in healthy humans reduces sympathetic nerve activity. Brain Stimulation. 2014;7(6):871-877.
- Badran BW, Mithoefer OJ, Summer CE, et al. Short trains of transcutaneous auricular vagus nerve stimulation (taVNS) have parameter-specific effects on heart rate. Brain Stimulation. 2018;11(4):699-708.
- Geng D, Liu X, Wang Y, Wang J. The effect of transcutaneous auricular vagus nerve stimulation on HRV in healthy young people. Oathes DJ, editor. PLOS ONE. 2022 Feb 10;17(2):e0263833.
Share via:


