A comprehensive review of how VNS devices restore gut function by addressing nervous system dysregulation, with expert rankings of the top 4 certified options.

Irritable gut affects an estimated 5-10% of the global population, causing debilitating digestive symptoms that disrupt daily life. For many, Small Intestinal Bacterial Overgrowth (SIBO) underlies these symptoms. Unlike simple food sensitivities or stress, irritable gut and SIBO represent fundamental gut-brain axis dysfunction that disrupts digestion, gut motility, immune response, and overall well-being.
Recent neuroscience research has identified a critical mechanism: vagus nerve impairment. When this principal nerve controlling your digestive system demonstrates reduced activity, your body loses its capacity to regulate gut motility appropriately, control inflammation, and maintain healthy gut bacteria balance.
This guide examines the relationship between vagus nerve function and irritable gut /SIBO symptomatology, and evaluates the leading vagus nerve stimulation (VNS) devices that may help restore digestive balance and functional capacity.
Symptoms of Irritable Gut & SIBO
Irritable gut is characterized by recurrent abdominal pain associated with changes in bowel habits, occurring at least one day per week for the past three months. SIBO involves excessive bacteria in the small intestine, often driving irritable gut symptoms. Common manifestations include:
Digestive symptoms:
- Abdominal pain or cramping, often relieved by bowel movements
- Bloating and visible abdominal distension, particularly after eating
- Gas and flatulence, sometimes excessive and embarrassing
- Diarrhea, constipation, or alternating between both
- Urgent need to have bowel movements
- Feeling of incomplete evacuation
- Mucus in stool
Food-related symptoms:
- Food sensitivities or intolerances (especially FODMAPs, gluten, dairy)
- Nausea, particularly after meals
- Acid reflux or heartburn
- Early satiety (feeling full quickly)
- Post-meal fatigue or "food coma" effect
Systemic symptoms:
- Brain fog and difficulty concentrating
- Tiredness unrelated to sleep quality
- Headaches
- Anxious thoughts or depressive states (often worsened by digestive issues)
- Sleep disturbances
- Body aches and joint pain
Autonomic dysregulation:
- Symptoms worsen with stress
- Temperature sensitivity affecting digestion
- Heart palpitations or rapid heartbeat with digestive flares
- Dizziness, particularly after eating
- Difficulty relaxing or feeling "wired and tired"
The functional impact extends beyond physical discomfort: inability to eat socially, planning life around bathroom access, dietary restrictions that isolate you, lost work productivity, anxious thoughts about symptom flares, and significant reduction in quality of life metrics.

Irritable Gut & SIBO Self-Assessment
Evaluate the symptoms you experience with regularity:
Digestive Function
- Abdominal pain or cramping at least once per week
- Bloating that worsens throughout the day
- Bowel movements that alternate between diarrhea and constipation
- Urgent need to use the bathroom, sometimes with little warning
- Gas or flatulence that feels excessive
- Feeling like you haven't fully emptied your bowels
Food Responses
- Certain foods consistently trigger digestive symptoms
- Bloating or pain within 1-2 hours of eating
- Nausea after meals, especially larger ones
- Avoiding social eating due to fear of symptoms
- Restricted diet due to food sensitivities
- Unexplained weight loss or difficulty maintaining weight
Symptom Patterns
- Symptoms improve temporarily after bowel movements
- Stress or anxious thoughts makes digestive issues worse
- Symptoms have persisted for at least three months
- Conventional solutions (diet changes, probiotics) provide incomplete relief
- Multiple food elimination diets tried with limited success
Systemic Impact
- Brain fog or tiredness after eating
- Sleep disrupted by digestive discomfort
- Mood changes (anxious thoughts, depressive states) related to gut symptoms
- Planning daily activities around bathroom access
- Social isolation due to dietary restrictions or symptom unpredictability
Autonomic Symptoms
- Feel stuck in "fight-or-flight" mode
- Difficulty relaxing even when trying to rest
- Heart races or pounds during digestive flares
- Temperature changes affect your digestion
- Shallow breathing or feeling of chest tightness
Diagnostic History
- Diagnosed with irritable gut by a gastroenterologist
- Tested positive for SIBO via breath test
- Endoscopy or colonoscopy ruled out structural problems
- Standard medications (antispasmodics, laxatives, anti-diarrheals) provide minimal relief
- Symptoms began or worsened after illness, antibiotics, or major stress
If you identify with 10+ items, particularly in Digestive Function, Food Responses, and Symptom Patterns categories, you may have irritable gut and SIBO related to vagus nerve dysfunction and impaired gut-brain communication.
Vagus nerve stimulation may warrant discussion with your healthcare provider as an adjunctive approach.
The Vagus Nerve Connection
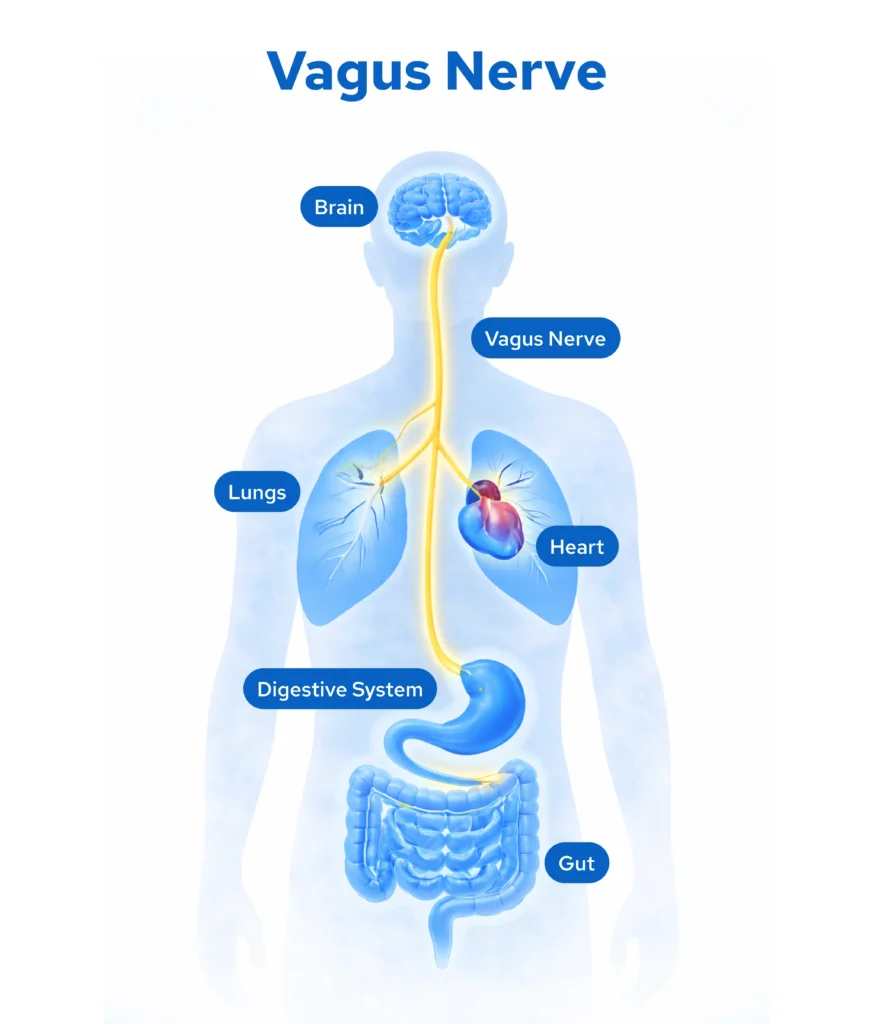
What Is the Vagus Nerve?
The vagus nerve (cranial nerve X) is the longest nerve in your body, traveling from your brainstem down through your neck to innervate most of your digestive tract. It mediates critical gut functions:
- Gut motility (the wave-like contractions that move food through your system)
- Digestive enzyme and acid secretion
- Gut barrier integrity (preventing "leaky gut")
- Inflammatory regulation (controlling immune responses in the gut)
- Microbiome balance (influencing which bacteria thrive)
- Gut-brain communication (sending signals about hunger, fullness, and pain)
The Two-Mode System

Your autonomic nervous system operates through two complementary divisions:
- Sympathetic (stress response): Slows digestion, redirects blood flow away from the gut, increases gut sensitivity to pain, promotes inflammation, activated during stress or perceived threat.
- Parasympathetic (rest-and-digest): Controlled predominantly by the vagus nerve, stimulates digestive secretions, promotes gut motility, reduces inflammation, supports healthy gut bacteria, and calms pain signals.
Healthy digestive function requires appropriate parasympathetic (vagal) activity. However, chronic stress, infection, antibiotics, or immune activation can impair vagal tone, creating sympathetic predominance that disrupts your entire digestive system.
How Vagus Nerve Dysfunction Causes Irritable Gut & SIBO

When your vagus nerve demonstrates reduced activity (low vagal tone):
- Impaired gut motility: Without appropriate vagal signaling, the muscular contractions that move food through your digestive tract slow down. This creates stagnation in the small intestine, the perfect environment for bacteria to overgrow where they shouldn't be (SIBO). Slow motility also means food ferments longer, creating gas, bloating, and abdominal discomfort.
- Disrupted migrating motor complex (MMC): The vagus nerve controls the MMC, a "cleansing wave" that sweeps through your intestines between meals, clearing out bacteria and debris. With vagal dysfunction, this cleaning mechanism fails, allowing bacteria to accumulate and proliferate in the small intestine.
- Increased inflammation: The vagus nerve activates the cholinergic anti-inflammatory pathway, releasing acetylcholine that calms immune responses in the gut. When vagal activity is low, gut inflammation goes unchecked. This damages the intestinal lining, increases permeability ("leaky gut"), and amplifies food sensitivities and immune reactions.
- Microbiome dysbiosis: Vagal tone directly influences which bacterial species thrive in your gut. Low vagal activity creates an environment where inflammatory bacteria overgrow while beneficial species decline. This dysbiosis drives bloating, gas production, and systemic symptoms like brain fog and tiredness .
- Heightened pain sensitivity (visceral hypersensitivity): The vagus nerve normally modulates pain signals traveling from the gut to the brain. With impaired vagal function, even normal digestive sensations feel painful. This explains why irritable gut users experience severe pain from gas or contractions that wouldn't bother someone with a healthy vagal tone.
- Chronic stress perpetuation: Digestive symptoms create anxious thoughts ("When will I have a flare?"), which further reduces vagal activity. This creates a vicious cycle: low vagal tone worsens gut symptoms, gut symptoms increase stress, stress further suppresses the vagus nerve. Without intervention, this cycle becomes self-perpetuating.
The Scientific Evidence
Published research establishes clear relationships between vagus nerve dysfunction and irritable gut /SIBO pathophysiology:
- Gut-brain axis dysfunction: Studies document that irritable gut users exhibit distinct autonomic abnormalities consistent with impaired vagal control of digestive function. Heart rate variability parameters (validated biomarkers of vagal tone) are markedly reduced in irritable gut users compared to healthy controls, indicating parasympathetic withdrawal.
- Vagal nerve activity predicts gut motility: Research demonstrates that individuals with higher vagal tone have significantly faster intestinal transit times and healthier gut motility patterns. Conversely, those with low vagal activity show delayed gastric emptying and small bowel transit, key contributors to SIBO development.
- Scientific study evidence for vagus nerve stimulation in GI disorders: A comprehensive 2025 review analyzed 644 users with gastrointestinal disorders who received noninvasive vagus nerve stimulation. Results showed significant improvement in GI symptoms across all users , regardless of specific diagnosis. Users reported reduced abdominal pain, decreased bloating, and improved bowel regularity.
- Inflammatory bowel and functional GI disorders: Multiple studies have documented that vagus nerve stimulation reduces inflammatory markers (TNF-α, IL-6) in the gut while improving gut barrier function. This dual action (reducing inflammation and healing the intestinal lining) addresses core mechanisms driving both irritable gut and SIBO.
- Stress-gut connection: Research confirms that chronic stress suppresses vagal activity, directly contributing to irritable gut symptom flares. Studies show that interventions increasing vagal tone (including VNS) reduce stress-induced gut symptoms and improve resilience to dietary triggers.
- Microbiome modulation: Emerging research indicates that vagus nerve activity influences gut microbiome composition. Stimulating the vagus nerve promotes growth of beneficial bacteria (Lactobacillus, Bifidobacterium) while reducing inflammatory species. This mechanism may explain why VNS helps address the root cause of SIBO, not just suppressing symptoms but restoring bacterial balance.
- The mechanistic conclusion: Restoring vagus nerve function through targeted stimulation addresses the underlying gut-brain axis dysfunction driving irritable gut and SIBO (including impaired motility, chronic inflammation, microbiome dysbiosis, and pain hypersensitivity) rather than merely suppressing symptoms.
VNS Devices as a Solution: How They Work
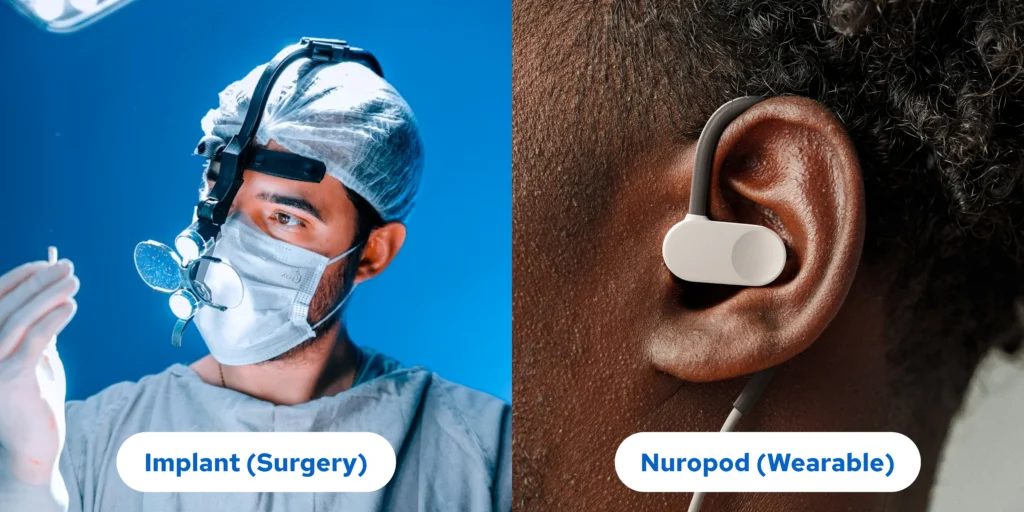
The Technology Revolution
Until recently, vagus nerve stimulation required invasive surgical procedures: implanting electrodes directly on the nerve through operations that carried surgical hazard, recovery time, and permanent device placement. This confined VNS therapy primarily to therapy -resistant depressive state cases where the benefits justified surgical intervention.
Today’s breakthrough changes everything.
Modern transcutaneous vagus nerve stimulation (tVNS) delivers the same therapeutic electrical impulses to the vagus nerve (facilitating restoration of appropriate gut-brain communication and digestive function) but completely non-invasively through the skin: no surgery, no implantation, no recovery period.
These advanced devices achieve remarkable effectiveness with an exceptional safety profile, operating through precisely positioned electrodes at two accessible locations
- Cervical (neck): Targeting the cervical branch of the vagus nerve near the carotid artery where the nerve courses superficially beneatht. But the neck site stimulates indiscriminately, activating surrounding muscles and nearby nerves alongside the vagus, making precise delivery difficult. It requires holding the device against the throat throughout each session, ruling out hands-free use. And compared to auricular stimulation, the cervical approach has a fraction of the clinical research behind it, with far less consensus on its safety and long-term efficacy.
- Auricular (ear): Targeting the auricular branch of the vagus nerve innervating the ear, the only place where the vagus nerve reaches the body's surface.
This represents a fundamental shift: vagus nerve stimulation therapy that was once confined to operating rooms is now available for daily home use, with scientific-grade precision and very low surgical hazard.
Mechanism of Action
When precisely calibrated electrical impulses reach the vagus nerve, they initiate a cascade of gut-healing responses:
- Restoration of gut motility: Stimulation activates vagal efferent fibers that control intestinal smooth muscle contractions. This restores the wave-like peristalsis necessary for proper food movement and reactivates the migrating motor complex (MMC) that prevents bacterial overgrowth.
- Inflammatory suppression: VNS triggers the cholinergic anti-inflammatory pathway, releasing acetylcholine that signals immune cells in the gut to reduce inflammatory cytokine production (TNF-α, IL-1β, IL-6). This calms gut inflammation and promotes intestinal healing.
- Gut barrier restoration: By reducing inflammation and modulating immune responses, vagus nerve stimulation helps repair tight junctions in the intestinal lining, addressing “leaky gut” and reducing food sensitivities.
- Microbiome rebalancing: Consistent vagal stimulation creates an environment that favors beneficial bacteria while discouraging overgrowth of inflammatory species. This helps restore healthy microbiome diversity, addressing SIBO at its root.
- Pain modulation: VNS enhances descending pain inhibition pathways from the brain to the gut, reducing visceral hypersensitivity. This means normal digestive sensations no longer trigger severe pain responses, significantly improving quality of life.
Clinical Parameters
Research-validated VNS protocols typically employ:
- Session duration: 30-60 minutes daily (allowing for sustained gut-healing effects)
- Intensity: Individualized to sensory threshold (perceptible but comfortable stimulation)
- Consistency: Daily application for minimum 8-12 weeks (gut healing and microbiome rebalancing require sustained intervention)
Expected Timeline
VNS promotes gradual gut healing rather than immediate symptom suppression:
- Week 1-2: Enhanced relaxation response during stimulation sessions, possible modest reduction in symptom severity, improved stress resilience affecting gut symptoms
- Week 3-4: Noticeable improvements in bloating and abdominal pain intensity, more regular bowel movements, reduced urgency, decreased food sensitivity reactions
- Month 2-3: Sustained digestive improvements, ability to reintroduce previously problematic foods, decreased reliance on restrictive diets, measurable reduction in symptom flares
- Month 3+: Restored gut motility and microbiome balance, functional capacity improvements, ability to eat socially without fear, enhanced quality of life metrics, potential to reduce or eliminate other medications
Safety Considerations
VNS using transcutaneous approaches is generally well-tolerated in scientific research. Potential transient responses may include:
- Mild tingling sensation at the stimulation site
- Temporary muscle tension in the neck region (cervical devices)
- Brief lightheadedness (typically resolves with protocol adjustment)
Important limitations: Not appropriate for individuals with cardiac pacemakers, recent acute cardiac events, pregnancy, or history of vagotomy. Healthcare provider consultation is essential prior to initiating any VNS protocol.
Top 4 VNS Devices for Irritable Gut & SIBO
#1: Nuropod

Price: $900 ($100 research subsidy available)
Type: Auricular (ear-worn)
Technology: AVNT™ by Parasym
Why #1:
- Most extensively validated: Supported by 50+ completed scientific studies and endorsed by 100+ global research institutions worldwide like Harvard, Stanford, Yale, the University of Pennsylvania, the University of Chicago Medicine and the University College London
- Demonstrated efficacy for gut disorders: Scientific study published in Advances in Neurology and Neuroscience documented 61% improvement in gastrointestinal function, brain fog, and pain in users with post-viral fatigue symptoms, with statistically significant results after just 10 therapy sessions (p < 0.0001)
- Independent certification: CE-marked device meeting rigorous safety and performance standards, third-party verified
- Scientific adoption: Used and recommended by 1000+ licensed healthcare professionals; integrated into institutional protocols; 4,000,000+ happy user sessions completed
- Evidence-based parameters: Stimulation protocols derived from research on gut-brain axis modulation, not proprietary guesswork
- Comprehensive support: 30-day evaluation period, scientific guidance resources, responsive technical support
Best for: Individuals seeking the most scientifically validated device, particularly those with irritable gut, SIBO, chronic gut issues, inflammatory bowel symptoms, or those prioritizing evidence over marketing claims.
#2: Truvaga Plus

Price: $544+ (device $499 + spray $45/year + potential subscription)
Type: Cervical (neck handheld)
Technical note: Shares core technology with gammaCore, an FDA-cleared device for headache/cluster headache (not gut disorders). Rapid parasympathetic effects. Straightforward protocol.
Considerations: Ongoing costs for conductive spray plus potential app subscription—verify pricing before purchase. Common side effects include muscle spasms, facial droop, lip pull, and headache. Not suitable for users with cardiac symptoms, pacemakers, or recent heart issues. Mobile app connectivity problems reported.
Best for: Those preferring cervical stimulation with FDA-cleared technology lineage (for headache, not irritable gut /SIBO) who can tolerate potential facial muscle spasm side effects.
#3: Pulsetto

Price: $350-$371 (device $269 + gel $81-$102/year)
Type: Cervical (hands-free collar)
Advantages: Hands-free wearable design. HSA/FSA eligible. 2-year warranty coverage.
Critical Limitations: No peer-reviewed scientific studies demonstrating efficacy for irritable gut or SIBO, only company press releases and retail testimonials. Frequent fit problems create inadequate nerve contact, especially with smaller necks. Users consistently report minimal to no improvement in gut symptoms compared to research-validated devices.
Not recommended for irritable gut /SIBO: The $200-350 price difference seems attractive until you calculate the real cost: months of continued digestive misery while using an unproven device. A $269 device that doesn’t work costs infinitely more than a $700 device that restores your gut function.
#4: Sensate

Price: $299-$349
Type: Chest-worn vibrotactile device (not true VNS)
Advantages: Comfortable pebble design worn on chest. Simple app interface with soundscapes. Lower price point. Can be used while performing other activities with a neck strap.
Critical distinction: Sensate does not directly stimulate the vagus nerve through electrical impulses like other devices in this comparison. Instead, it uses infrasonic vibrations and bone conduction placed on the chest, an indirect approach targeting general stress reduction rather than specific vagal nerve activation. While bone conduction at the ear has some research supporting vagal stimulation, Sensate’s chest placement lacks scientific substantiation for direct vagus nerve engagement. The mechanism is fundamentally different: actual VNS devices (like Nuropod, Truvaga, and Pulsetto) deliver calibrated electrical signals directly to accessible vagus nerve branches; Sensate delivers vibrations to your sternum hoping for downstream effects.
For Irritable gut /SIBO users : This matters significantly. Irritable gut and SIBO require restoration of measurable gut function, improved motility, reduced inflammation, microbiome rebalancing, and pain modulation. General relaxation devices may help with stress management but do not address the underlying vagal dysfunction and gut-brain axis dysregulation driving digestive symptoms. No scientific studies demonstrate Sensate’s efficacy for irritable gut, SIBO, or any gastrointestinal disorders; only company-funded studies showing general stress reduction in healthy volunteers.
Best for: Those seeking a general relaxation and stress management tool rather than targeted vagus nerve stimulation for gut dysfunction. Not recommended for individuals prioritizing evidence-based irritable gut /SIBO solution.
Conclusion: Nuropod offers the most comprehensive scientific validation, proven efficacy for gastrointestinal dysfunction including irritable gut symptoms, independent regulatory certification, and optimal balance of research foundation and practical application for those prioritizing evidence-based gut healing outcomes.
Take Action
Irritable gut and SIBO related to vagus nerve dysfunction represent treatable symptoms . Your gut-brain axis possesses the capacity for healing and restoration of healthy digestive function.
With support from 50+ completed scientific studies, CE-marking certification, and 4M+ happy user sessions completed, Nuropod provides scientifically validated potential for restoring gut-brain balance and functional digestive capacity.
This information is provided for educational purposes. VNS devices are not intended to diagnose, treat, cure, or prevent any disease. Individuals with irritable gut or SIBO should work with qualified healthcare providers to develop comprehensive management strategies. Always consult your physician before beginning any new intervention.
Share via:


